If somebody were to ask me “What’s the most important marketing skill in 2020?” I would have to answer “empathy.” On a global level, just listening to the bad news roll in every morning, people are stressed, anxious, outraged, frustrated, and depressed. Currently, a third of Americans are showing signs of clinical anxiety and depression. The rates of mental stress are higher among younger adults, with many researchers worried about suicide increasing among teens.
Remember this the next time you see a video of somebody flipping their lid at a Costco on TikTok. “Retail rage” is yet another trend that’s grown since the pandemic. Objectively, we might see somebody throwing a tantrum in a store and think of them amazingly petty. But the big picture is that people are barely holding it together right now, to the point where they can keep their stress carefully bottled up, hidden away, until McDonald’s forgets the cheese on their burger, and then that’s the breaking point. All the stress comes out at once.
It’s a sensitive time and businesses are looking at their marketing departments to help them get through it. With revenue down, the pressure is on marketing to engage existing customers, identify and expand into new markets, and protect brand reputation above all else.
If you want to be successful in the pandemic economy, marketers need to focus on the people. Your customers should be at the forefront of your mind and inform all of your marketing decisions. This is an overarching theme of the new pandemic marketing playbook. So, let’s take a look at what people-first marketing looks like:
The New Pandemic Marketing Playbook
Communication Strategies
Old and busted: Paying lip service to customer-first standards through bland, canned, corporate messages.
New and hot: The human touch.
This Forbes article meanders about before getting to the point that social media has become the most important communication channel for both consumers and companies.
“Businesses, as well, have found renewed value. We’ve seen a 15-20% increase in posts from our 18 million users, as companies reach out to customers and employees. Moreover, how they use social media is changing. Our data shows marketing and ads have given way to direct engagement—one-on-one interaction with other people.”
They point to the Twitter feed of Steak-Umm (a frozen steak brand) as an example of humanized marketing. They get what people are going through, and have been sharing messages that we can all relate to, be comforted by, and laugh at. It’s not limp corporate-speak. They’re willing to take a position and even poke fun at themselves a bit.
Hello, post-modernist, 4th-wall-breaking humor! We haven’t seen you since the swinging ’60s, welcome back! Note that the post got 98 retweets and over 1K likes. Is your branded social media marketing campaign doing this well?
Besides the point of humor, we’re advocating that marketing messages include these ingredients in the formula:
- Understanding your customers’ challenge: Don’t just tell, show
- Embracing the person: Love your customer’s quirks, personalize for them
- Segment content: One catch-all marketing campaign isn’t cutting it right now
- Plain facts: Strive for frank sincerity and transparency as much as you can
The more relevant your product or service is to current customer needs, the more you should emphasize this in your marketing. Give customers the impressions that you made this product for them, that you understand their needs, and designed the product around their needs.
Marketing Channels
Old and busted: Sticking to just one channel.
New and hot: Omnimarketing.
“Omnimarketing” means broadcasting your message across the spectrum of digital channels. People are spending more time online than ever, and you need to reach your audience on the various channels they use daily. Craft your message so that it’s appropriate for the channel and relevant to what they do there.
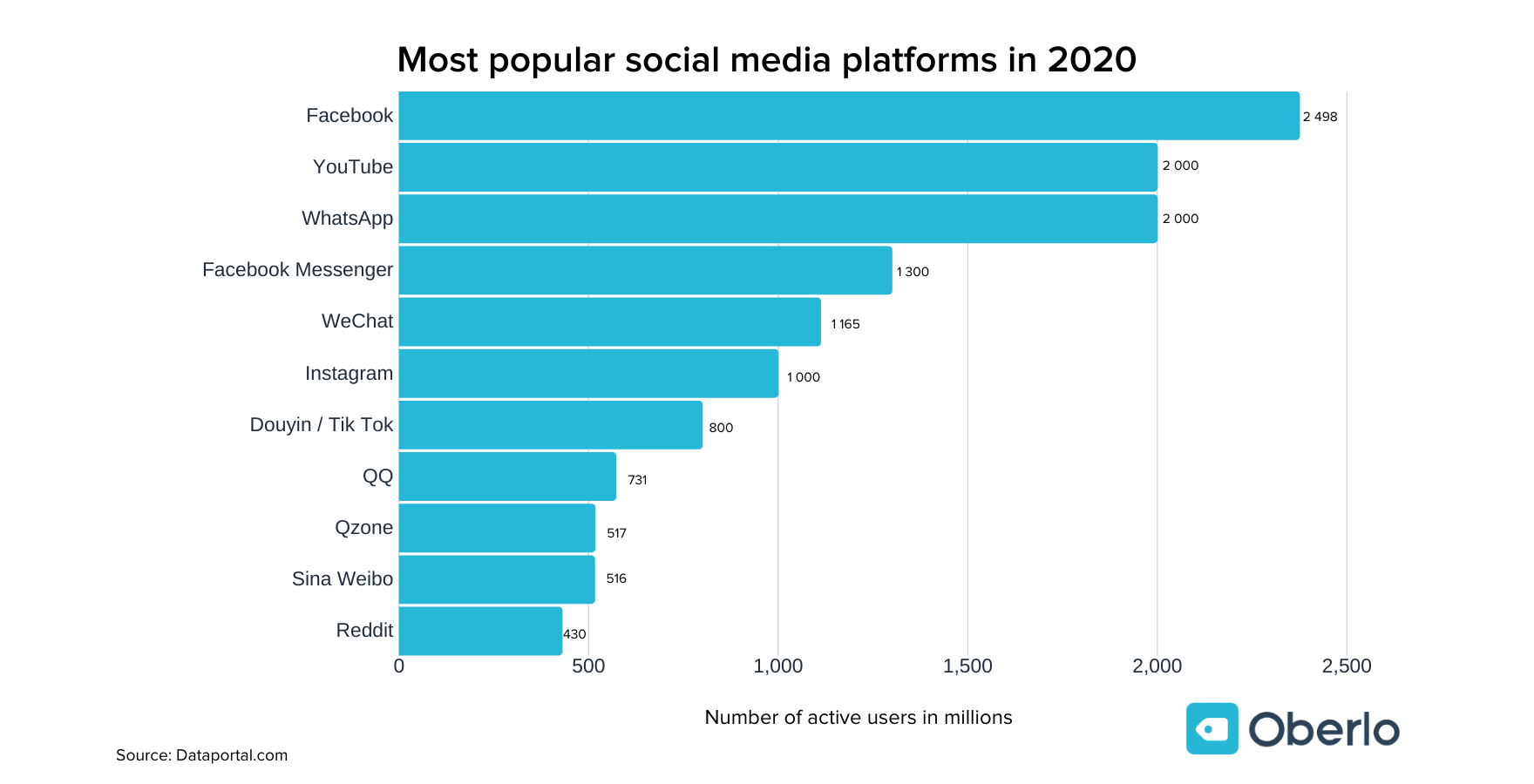
Facebook is certainly dominant, but there are plenty of hipsters who won’t use Facebook simply because it’s too crowded, noisy, and they don’t trust Zuckerberg. YouTube is also huge, but there are still market segments loyal to Vimeo and Pluto TV. If you’re wondering what “QQ” is, that’s Tencent QQ, the most popular media web portal in China and the world’s 5th-most visited website by Alexa stats.
Granted, your market may not be ideal for China, but it goes to show that whole social media subcultures can be huge and still unknown to much of the world.
One new rising star on social media is NextDoor, a neighborhood-based kind of Facebook. Linked-In, the “Facebook for professionals,” is often overlooked. And don’t look now, but marketers are starting to creep into Reddit and its multimedia-focused sister site Imgur. Some of us, especially those of us in the digital marketing industry, hang out on multiple platforms throughout the day. Clicking through tabs to see what’s going on in the various social media channels has replaced leafing through the newspaper over breakfast.
Beyond the social media channels, you should consider the other channels your customers use. What websites do they frequent? Where do they get their news? Running display ads on those channels is a good way to remind them of your brand. What about Google Ads? Targeting the keywords they use will make sure your brand is found when they head to a search engine.
We still have to tackle email marketing. Your website should be generating leads through forms for special offers, blog subscriptions, or content like eBooks, webinars, and white papers. Once you have their email address, you can nurture them with relevant, helpful content that’s personalized to them. Give them the information they need to make informed decisions.
With uncertainty still the norm, email nurturing is an essential part of the new digital marketing playbook. People are hesitant to commit to purchases now and must be nurtured until they’re ready.
We have a fresh tutorial on lead generation tools including email marketing and landing pages.
Your Website Experience
Old and busted: Static sites that haven’t been updated since the Bush administration.
New and hot: Dynamic, easy-to-use websites optimized for mobile.
We harp on Google a lot in digital marketing, but that’s what you do when it’s the world’s leading search portal. Consequently, Google has begun to have more and more jurisdiction over what sites get traffic on the web.
Google Webmaster Guidelines have been focusing on:
- Updated, secure websites
- Mobile-friendliness
- Fast and efficient page loads
- Uncluttered user interface (UI)
- Responsive design
- Clear, informative, useful content
Gradually over time, Google’s standards have moved from “suggested for best results,” to “we now insist you do this,” and finally to “do this or we won’t list your site.” Google has been rolling out a new, united standard: Core Web Vitals.
Everybody panic! No, actually, Core Web Vitals are just the encapsulation of the traits we just listed, but with a heavier focus than ever on mobile-friendly content.
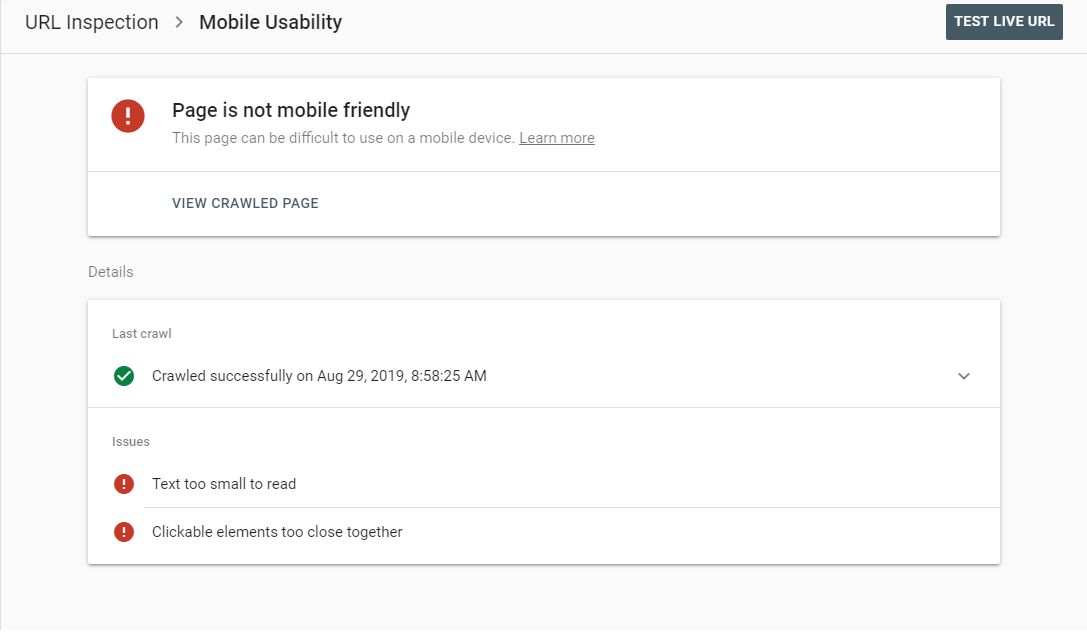
This means not just being fast and fitting the size of a phone screen, but having the interface optimized so that the text is large enough to read on a phone and the links can be comfortably tapped with the average finger (or stylus). It means not having a cluttered, busy interface with too many pop-ups (“interstitials,” as Google calls them) that can be difficult to navigate with a thumb.
Google is echoing Blizzard Entertainment right now: “Do you guys not have phones?” Yes, of course, we have phones, but nobody gets work to any significant degree done on a phone. We work with laptops, which gives us a blind spot for phones, which is why Google has to say “pay attention to how it works on a phone.” Laptop to produce content, phone to consume content.
Even without Google (can we even imagine such a world?), Core Web Vitals is about nothing more than “have an outstanding website experience that people love to use.” We all wanted to do that anyway, right?
Advertisement Targeting
Old and busted: General ad campaigns served to everyone.
New and hot: Laser-focused audience targeting.
Above, we mentioned email marketing, which allows you to capture the part of the audience that visits your website, doesn’t initiate business with you on the spot, but shows some interest in the future. These email addresses are useful for more than just email marketing, however. You can take your list of leads and plug them into Facebook or Google Ads to form a custom audience.
Our full in-depth guide to Facebook custom audiences is here.
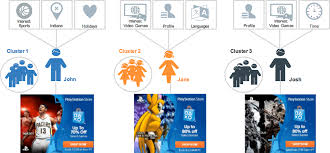
You can do all kinds of tricks with a custom audience:
- Target the people who have visited your site and signed up for your newsletter
- Target a “cloned audience” whose demographics match your newsletter audience
- Create a reverse-targeted audience for everybody who has never visited your website
You see custom audiences in action all the time with the ads you see online. Visit a site, buy a product, and mysteriously, an ad for a similar product will appear on an unrelated site you visit later. Tracking user behavior like this has become the norm. Sometimes it feels like an eerie AI cyber-presence is reading your mind.
You can use ad targeting to create custom ads directed at groups such as former customers, or leads who came close to a conversion but didn’t pull the trigger. You can show special promotional offers to re-engage them. Remind them if they started an enrollment process or left an item in a shopping cart app without completing the transaction.
You should use audience targeting the way a chef uses their strongest spice: Enough to have an effect without overwhelming it. There is a little backlash over intrusive data mining out there, including users who will turn on privacy settings and use tools that don’t track you, such as DuckDuckGo. Serious privacy advocates will turn to VPNs to hide their activity. But the backlash has started dying down. Just try to keep your ads as non-intrusive as possible, without making the user feel like they’re under a microscope.
Customer Interaction
Old and busted: Face to face contact.
New and hot: More remote, virtual, and digital interactions, please.
Of course, our whole website, and every blog post on it is about digital marketing, so all these remote, online interactions are already familiar territory. But the pandemic has put more focus on digital customer service than ever before. Every close encounter is one more transmission risk, so the more contact we limit the better—at least until COVID-19 blows over.

You want to be sure customers can interact with you over:
- text
- phone
- social media
- your website
In addition, chatbots offer a smarter, more interactive customer service experience as compared to a plain form on your website’s landing page. They can be customized with a script to help the customer navigate the most common interactions with your business. Younger users especially are more prone to interact with chatbots. We think chatbots don’t get a fair rap because people associate them with those voice-based phone bots you have to yell everything at three times. Chatbot technology has improved tremendously and help people quickly get the information they need.
Multimedia
Old and busted: The Internet is a media, right?
New and hot: Living on Video!
The mobile era has had the fortunate side effect of popularizing online video content. Video accounts for a huge chunk of the market now, with YouTube being the second-most visited website right after Google.
Video and audio content has defined the 2010s web experience like nothing else. Whether it’s following a favorite gamer on Twitch, binge-watching a TV series on Netflix, or keeping up with podcasts on Spotify, online consumers are plugged into multimedia.
Due to all of the above-mentioned factors—customers wanting less personal interaction but also more engaging media—video content marketing has come to be one of the most important channels in the digital business world. Just as with blog-based content marketing, your video marketing should have some other goal besides direct advertisement. Such as to:
- Entertain: People are seeking distractions and anything that will make them laugh.
- Be helpful: Help them solve problems, learn new skills, or accomplish their goals.
- Inspire or motivate: Share just a “thought of the day” or “mental health break” message.
- Provide industry updates and insights: Hot developments in your industry or new trends.
Video content humanizes a brand and lets those couch-bound, quarantined users, who are working from home or attending remote university, hear another human voice. At the very least, video content provides an entertaining distraction.
Closing Thoughts…
Take this one word home with you: “Empathy.” We see and hear stories every day where consumers are complaining about the lack of empathy in commercial or governmental contexts. People need empathy right now, and it’s the secret ingredient that will make your digital marketing strategies successful. So, reach out and listen to people and give them a comforting presence at your digital hearth. A little tender touch right now goes a long way!

